About nappy rash
Nappy rash is a very common skin condition. It happens when the skin on your child’s bottom is damaged and irritated.
The main cause of nappy rash is wearing a wet or dirty nappy for too long. This is because your child’s skin can be irritated by a chemical called ammonia, which is in wee and poo. The dampness of wee and poo can be irritating too.
Other things that can cause nappy rash or make it worse include:
- friction between the nappy and the skin
- plastic pants – they stop air circulating normally and keep the nappy area damp
- soaps, detergents, fragrance and plant or food products left on the skin from bathing or left on cloth nappies from washing
- a chemical called methylisothiazolinone, which is in some disposable baby wipes
- conditions like eczema, psoriasis, thrush or impetigo.
Nappy rash is less common in babies who are breastfed, because their poo is less irritating. And it’s more common in babies who wear cloth nappies, because cloth nappies are less breathable and absorb less moisture than disposable nappies.
Symptoms of nappy rash
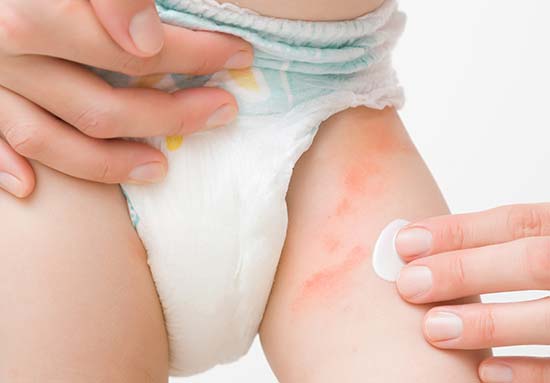
The skin on your child’s bottom and genitals will look inflamed and sore. On children with dark skin, the inflammation might look brown, purple or grey. On children with light skin, the inflammation might look red.
Some areas of skin might be raised or swollen, and there might be breaks in the skin. These breaks are called ulcers.
Skin folds aren’t usually affected because wee doesn’t get into them. But nappy rash might sometimes go up onto your child’s tummy or spread up towards your child’s back.
The rash can be uncomfortable and even painful, which can make your child irritable.
Medical help: when to get it for children with nappy rash
You should take your child to the GP if your child:
- has nappy rash that hasn’t improved after a week, even when you use the treatment below
- has blisters, crusts or pimples
- is upset and isn’t sleeping
- has an unexplained fever
- has nappy rash that’s spreading
- has inflammation, swelling or a scab at the end of their penis.
Diagnosing nappy rash
Your GP will talk to you about your child and look at their skin to diagnose nappy rash. Sometimes the GP might take a swab to identify any thrush or bacteria on the skin.
Treatment for nappy rash
The aim of nappy rash treatment is to repair the damaged and irritated skin and protect it from any dampness and friction that might cause more damage.
Change your baby’s nappies frequently
Frequent nappy changes keep the nappy area dry and give your child’s skin a chance to heal. Check your child every hour or so to see whether their nappy is wet or soiled. Change wet or soiled nappies straight away.
Clean your baby’s skin
Use lukewarm water and cotton wool or a light cotton cloth to gently clean your child’s skin after each nappy change.
When you bath your child, use a gentle, soap-free wash. Pat your child’s skin dry, and gently apply a simple moisturiser.
Use a protective cream after each nappy change
Apply a simple, cheap barrier cream at every nappy change. You could use a zinc cream or a petroleum jelly like Vaseline. You can get these creams from a supermarket or your pharmacy without a prescription.
You should apply the cream thickly enough to create a barrier that stops wee and poo from getting onto the skin. You’ll know you’re putting the cream on thickly enough if you can still see some of the cream at the next nappy change.
Nappy-free time
Air your child’s bottom for as long as possible every day. Let your child play or sleep without their nappy – just put a towel underneath them.
To allow air to circulate freely and reduce friction, you could also fasten your child’s nappy loosely or use a larger nappy.
Use disposable nappies
Disposable nappies absorb more moisture. If you regularly use cloth nappies, consider switching to disposable nappies for a short time until the rash has healed. Avoid plastic overpants if you’re using cloth nappies.
Wash and rinse cloth nappies thoroughly
Get rid of soap residue on cloth nappies by rinsing well in fresh water, particularly after using bleach-based detergents. Make sure that nappies are dry before using them again.
Diet
Try to give your child fluids earlier in the evening to minimise night-time nappy wetting.
Highly acidic foods like citrus fruits, strawberries, pineapple, tomatoes and tomato-based products can make nappy rash worse. During episodes of nappy rash, you could consider reducing the amount of these foods and drinks in your child’s diet.
Medications
For severe nappy rash or nappy rash that won’t go away with simple measures, your GP might recommend using weak corticosteroid creams or ointments like hydrocortisone 1%. These are safe to use for a little while under the supervision of your doctor. Always follow the instructions on the packet when putting these creams on your child.
Your GP might also prescribe other creams or ointments if your child has a secondary infection with bacteria or fungus (thrush).
Complications of nappy rash: thrush and other infections
It will take weeks for your child’s skin to repair itself. While this is happening, your child’s skin might be more easily irritated.
Your child might also be more likely to get other infections like thrush. Thrush looks like bright, inflamed patches with clearly defined borders in the nappy area. You might also see a lot of dots or pus-filled bumps (pustules) beyond the outer edge of the rash. Thrush can affect the skin folds too.
Treat thrush with an antifungal cream prescribed by your GP. Thrush can take longer to clear than regular nappy rash and often comes back. Treatment can take a long time.
Nappy rash also increases the risk of urinary tract infection and vaginal infections in girls. This is why it’s important to treat nappy rash and prevent it if you can.
Prevention of nappy rash
Prevention is always better than treatment.
You can reduce the chance of your child getting nappy rash by keeping their nappy area clean and dry. Change your child’s nappy frequently and air their bottom as often as you can.
Protective barrier creams like petroleum jelly or zinc and castor oil can help keep your child’s skin in good condition.