About warts
Warts are a skin infection caused by the human papillomavirus (HPV).
Warts spread through direct, repeated skin contact with people who are already infected by HPV. They can also spread through contact with objects that are contaminated with the virus, like towels or nail clippers.
HPV is more likely to infect skin that’s broken or cracked – for example, when the feet are sweaty and soggy.
Not all people who come into contact with warts develop them. This is because people have varying levels of immunity to warts.
Warts are common in school-age children and teenagers. Children with eczema and a weakened immune system because of a medical condition or medical treatment also have a higher chance of developing warts.
Symptoms of warts
Warts usually appear gradually.
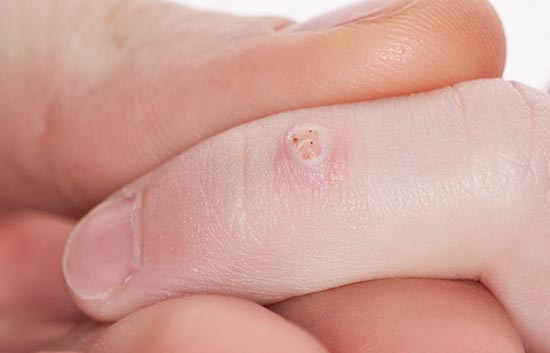
Common warts grow anywhere but most often on the arms, hands, fingers, legs, feet and face. They’re usually pinkish or flesh coloured and have a raised, rough appearance. They have a distinct border with the skin and might have tiny dark dots inside them. They might look like a little cauliflower on the skin.
Plantar warts grow on the soles, toes and heels of the feet. They often look flat on top where you walk on them because they’ve been pushed into the skin. They can be uncomfortable.
Plane warts are small, almost flat and flesh coloured. They often grow in groups over the back of the hands or the face. They’re more common in children than adults.
Genital warts occur around the groin region. They’re not common in children.
Mosaic warts are warts that have grouped together to make a pattern that looks like mosaic tiles.
Warts are generally painless – except for plantar warts, which can be painful to walk on.
Medical help: when to get it for children with warts
You should take your child to your GP if warts:
- are on your child’s face, feet or genitals
- look infected – the area around the wart might be swollen, warm and red on light skin, or brown, purple or grey on dark skin
- are painful or bleeding
- have been there for a long time
- aren’t responding to treatment
- are spreading around your child’s body
- are bothering your child because of the way they look.
You should also take your child to see the GP if your child has a growth on their skin and you’re not sure what it is.
Treatment for warts
Around half of warts go away by themselves within 6 months. Nearly all will go away within 2 years.
If the wart doesn’t clear up by itself or your child is bothered by the pain or the appearance of a wart, your GP can tell you the best way to get rid of it.
You can do some treatments at home. Other treatments need to be done by your GP. For more specialised treatments, the GP might refer your child to a dermatologist.
Wart paint
Many people use wart paint to get rid of warts. Wart paints are usually a combination of acids that destroy skin cells. Although wart paints are slow to work, they’re relatively painless compared with other treatments.
You can buy wart paints at your local pharmacy and apply them at home. If you need a stronger solution, your GP can give you a prescription.
Here are steps to follow if you’re using wart paint:
- Soak the affected area in warm water for 5-10 minutes. Treating the wart after a shower can help with this step.
- Rub the wart with a nail file, emery board, pumice stone or even clean, unused sandpaper.
- Put the paint on the wart, avoiding the healthy skin around it. If you’re using a prescription-strength paint, you might need to cover the surrounding skin to protect it.
- Let the paint dry. Cover the area with tape or strong, waterproof sticking plaster.
You usually need to use wart paint every day, and it can take many weeks to work.
Liquid nitrogen
Liquid nitrogen works more quickly than wart paint, but it’s painful.
Your GP will spray the liquid nitrogen directly onto the wart. Sometimes they might put it on with a cotton bud. This freezes the top layers of the wart, which destroys the affected tissue and releases the virus into the bloodstream. The body’s immune system then finds and fights the virus.
The treated area might be painful for minutes or even hours. A crust or blister will form and then drop off within a week.
You usually need several applications of liquid nitrogen a few weeks apart.
Liquid nitrogen might be combined with other treatments.
Burning and laser
Burning and laser wart removal treatments are done under local anaesthetic. Both treatments can leave scars, which might make it difficult to treat the wart if it comes back in the same spot.
Immunotherapy
Immunotherapy involves putting differing concentrations of allergic solution on the wart. This creates a type of skin inflammation, which causes the immune system to kill off the wart. This treatment takes time and can be very itchy.
Imiquimod
This is usually a treatment for genital warts rather than common warts. Sometimes it’s useful for small plane warts in areas that are hard to treat, like the face.
Prevention of warts
If your child has a wart, it’s a good idea to explain to your child that picking at the wart might cause more warts. This is because the HPV virus can spread to different parts of the body on fingers and fingernails.
Also encourage your child not to chew on warts. Chewing on a wart might lead to warts appearing on your child’s lips or face a few months later.
Make sure that your child doesn’t share treatments with other people in your house. This means not sharing nail clippers, wart paint, pumice stones and files.
Make sure that your child wears thongs or sandals in public showers or changing rooms. These are places where they could catch plantar warts.
HPV vaccination can protect young people from genital warts. HPV vaccination is part of the Australian National Immunisation Program for teenagers and is available free to all children aged 12-13 years.
Unless your child repeatedly touches another child’s warts, they’re unlikely to get infected.