About ringworm or tinea
Ringworm, or tinea, is a fungal skin infection.
Children most often get ringworm from young animals, like kittens and guinea pigs. They can also pick it up through contact with infected people and contaminated objects, including playground equipment, carpet, shower floors, brushes, clothing and towels. Soil contains ringworm too.
There are different names for ringworm, depending on where it is on the body:
- Tinea capitis affects the scalp. It’s the most common fungal infection in children.
- Tinea corporis affects the body.
- Tinea pedis or athlete’s foot affects the feet. It’s common in teenagers, particularly those who swim or play a lot of sport.
- Tinea cruris or jock itch affects the groin. It’s common in teenagers and young men who play a lot of sport and sweat a lot. Most will also have tinea of the feet.
- Onychomycosis affects the nails. It’s a type of nail infection.
Symptoms of ringworm
Ringworm looks different depending on the body part that’s affected.
Children with tinea capitis get an oval or circular patch of itchy, scaly skin on their scalps. The patch might look red on light skin or brown, purple or grey on dark skin. Children might also get hair loss in the same area. A severe infection might cause swollen lymph glands in the neck and fever.
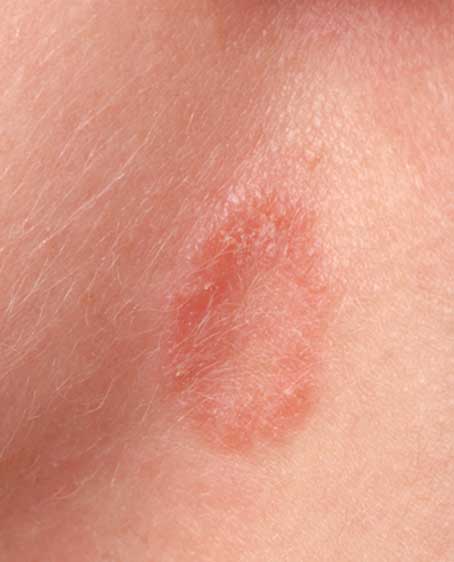
Tinea corporis first appears on the skin as a ring with a clear centre. The ring might look red on light skin or brown, purple or grey on dark skin. It might also have a lumpy, scaly or raised edge. It’s very itchy and can gradually get bigger. It sometimes spreads to other areas.
Tinea pedis causes white broken skin between the toes. It can also cause small blisters on the feet and a scaly rash that’s red on light skin or brown, purple or grey on dark skin.
Tinea cruris looks like a scaly rash in the groin area. The rash might look red on light skin or brown, purple or grey on dark skin. It’s often itchy. It most often happens on both sides of the groin at the same time.
Medical help: when to get it for children and teenagers with ringworm symptoms
You should take your child to the GP if your child has:
- several ringworm sores on their scalp or body
- painful sores
- sores or a rash that aren’t improving after a week’s treatment with antifungal cream
- sores or a rash that’s spreading despite treatment
- bald patches on their scalp
- a collection of pus on their scalp
- a fever and seems generally unwell.
Tests for ringworm
Your GP might use a special light to help diagnose ringworm. Or the GP might take skin scrapings from the area so the skin can be examined.
The GP might refer your child to a dermatologist.
Ringworm treatment
Ringworm usually gets better quickly when you treat it with antifungal creams, which you can buy over the counter at a pharmacy.
Ringworm treatment with antifungal creams usually takes several weeks to work. It’s best to keep applying the cream to the affected skin for a week after the rash has disappeared. This will remove all the fungus in the area and stop the ringworm coming back.
If antifungal creams don’t work or the ringworm is on your child’s scalp, your doctor might prescribe antifungal tablets.
If the ringworm is on the scalp, your child might have bald patches for a few months after it has cleared. Don’t worry, though – the hair will grow back.
Encourage your child to stop scratching the affected area. You could try distracting your child with music, play or reading. It might also help to put a cold cloth on the area.
It’s important to cover ringworm rash with clothing or a dressing to stop it spreading to other people.
Prevention of ringworm
To prevent ringworm, you can encourage your child to do the following:
- Avoid touching people who have a rash that looks like ringworm.
- Wash and thoroughly dry skin folds, including in the groin, under the arms and in between the toes.
- Avoid sharing towels, brushes, sheets, hats and combs with other people.
- Avoid walking in shared showers in bare feet.
Also, consult your vet if your pet has bald patches or sores, because this might be a source of ringworm infection.