About measles
Measles is caused by the measles virus.
Measles is very contagious. The virus spreads from person to person through coughing or sneezing.
Until recently there were almost no cases of measles in Australia because most children were immunised against measles as part of the National Immunisation Program. But more Australian parents are not immunising their children, so there are more cases of measles.
Measles symptoms
Symptoms usually start to appear 10-14 days after infection with measles virus.
The earliest symptoms look like those of a heavy cold – runny nose, fever, conjunctivitis and dry cough. Early in the illness children can have tiny white marks on the insides of their mouths. These are called ‘Koplik spots’.
The measles rash typically appears on the third or fourth day of the illness, starting behind the ears and along the hairline. It consists of small, irregularly shaped patches that spread over the face and neck during the first 24 hours. The patches might look red on light skin or brown, grey or purple on dark skin.
The patches later spread to the body, arms and legs. The patches might join to make the skin look blotchy.
The measles rash isn’t itchy.
Children usually start to feel better after 3-5 days. The rash starts to fade, and the fever goes down. Some children have skin peeling at this time.
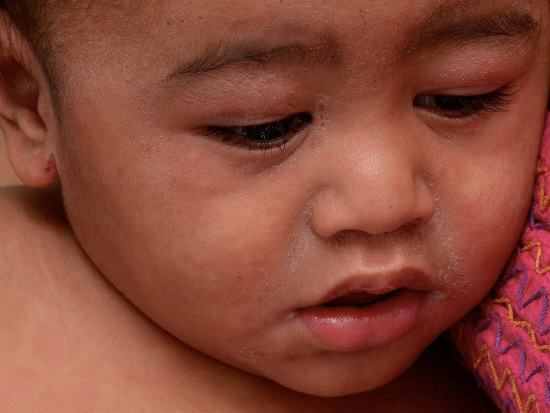
Image: measles on dark skin (source: DermNet)

Image: measles on light skin
Complications of measles
Measles can weaken the immune system, which means your child is more likely to get other infections like pneumonia and middle ear infections.
Encephalitis is another rare but very serious complication of measles.
If your child gets measles, they’re contagious from about one week before until about one week after the rash appears.
Medical help: measles symptoms or contact with measles
You should take your child to the GP if you’re worried your child might have measles. It’s a good idea to ring ahead in case your GP needs to take precautions to reduce the risk of measles spreading.
You should also see your GP if you or your child has been in contact with someone who could have measles, particularly if you or your child falls into a high-risk category. High-risk categories include:
- unimmunised children
- babies under 12 months of age
- children who have a weakened immune system because of health conditions like cancer
- pregnant women.
Take your child to your nearest hospital emergency department or call 000 for an ambulance straight away if your child has measles and:
- becomes drowsy
- gets a severe headache
- has difficulty looking at bright lights
- has difficulty breathing.
You know your child best. If your child seems unwell, seek medical attention.
Tests for measles
Your GP might do a blood test or nose swab to confirm that your child has measles.
Children and teenagers with measles or who’ve been in contact with someone with measles should avoid contact with other children and unimmunised adults until after they’ve seen a GP. Their GP will tell them whether they need to continue avoiding contact and for how long.
Treatment for measles
There are things you can do to ease your child’s symptoms:
- Give your child paracetamol or ibuprofen in recommended doses if your child has a fever that’s making them feel uncomfortable.
- Encourage your child to drink plenty of water and get plenty of rest.
- Try dimming the lights in your house if your child complains of sore eyes.
Don’t give aspirin to children under 12 years unless it’s prescribed by a doctor. Aspirin can increase the risk of Reye’s syndrome, a rare but potentially deadly condition. If you’re giving your child any over-the-counter medicines, check with your pharmacist or doctor to make sure these have no aspirin.
Prevention of measles
Immunisation is the best way to protect your child from measles.
As part of the Australian National Immunisation Program (NIP), your child gets 2 free measles immunisations. Your child needs both doses to have 99% immunity against measles. They’ll get these immunisations at:
- 12 months, as part of the MMR vaccine, which protects your child from measles, mumps and rubella
- 18 months, as part of the MMRV vaccine, which protects your child from measles, mumps, rubella and varicella (chickenpox).
Some parts of the world have high rates of measles. You should speak to your GP about whether your child needs additional travel immunisations at least 3 months before travelling to these areas.
Always wash your hands carefully if you’re caring for a child with measles.