About molluscum contagiosum
Molluscum contagiosum is a skin infection. It’s caused by a poxvirus.
It’s common in children and not dangerous.
Molluscum contagiosum spreads when children come into contact with an infected source. This could be another child, infected towels or contaminated water. Molluscum contagiosum can also spread when children touch the infected area and then touch different parts of their bodies.
Once someone gets infected with the virus, symptoms usually appear within 2 weeks, but they can take up to 6 months to appear.
Symptoms of molluscum contagiosum
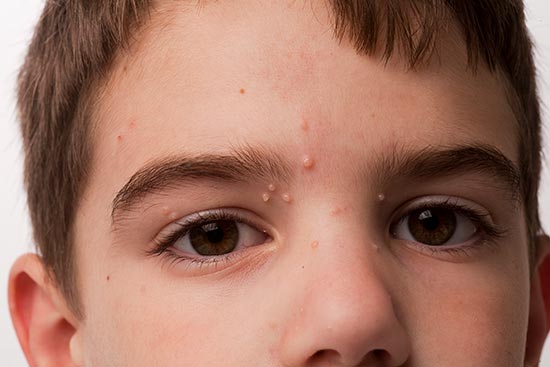
Molluscum contagiosum shows up as clusters of small, red, pink, flesh-coloured or pearly raised spots, often with a pit in the centre. The spots are usually 1-3 mm across, but they can get as big as 2 cm.
Molluscum contagiosum spots usually come up on the face, neck, inner thighs or buttocks, but they can come up anywhere.
Molluscum contagiosum spots aren’t painful, but they can be itchy. Eczema can develop in the surrounding skin.
Often molluscum contagiosum spots disappear without leaving a mark. But sometimes they can leave a pitted scar, like a chickenpox scar.
Does your child need to see a doctor about molluscum contagiosum?
If you think your child might have molluscum contagiosum, it’s a good idea to see your GP.
Molluscum contagiosum treatment
Many children don’t need treatment for molluscum contagiosum. The spots usually clear up by themselves, although this can take 6-9 months, or even a couple of years.
Doctors sometimes recommend treatment for molluscum contagiosum. This might be to:
- improve the way the spots look, particularly if the spots are somewhere obvious, like the face
- reduce the risk of spots spreading to other parts of the body, like the eyelids, lips or nose, which are harder to treat
- reduce the risk of spreading molluscum to other people
- reduce the risk of scarring – although some treatment options can cause scarring.
There are several treatments for molluscum contagiosum, but no treatment is totally effective. Your GP will help you decide what’s best for your child.
Your GP might suggest leaving sticky, waterproof tape on top of the spots for a few days. When you pull the tape off, the central core of the spots might pull off too. You can do tape stripping at home, and you might need to do it several times.
Sometimes the GP might suggest a retinoid cream. These can irritate your child’s skin, so it’s a good idea to talk through this option with your GP.
Imiquimod is another option. This cream can be expensive. It can also cause swelling and irritation before it heals.
Cantharadin is a lotion that causes blisters to form under the spots so that the spots lift off. Your GP will probably have to refer your child to a dermatologist for this treatment.
Other treatments include removing the central core of the spots with a needle, freezing the spots with liquid nitrogen, lasering the spots, or scraping the spots with a small surgical tool. Some children might find these treatments scary and painful. Some of these treatments might also lead to scarring.
If your child has eczema as well as molluscum contagiosum, your doctor will treat the eczema with an appropriate corticosteroid cream or ointment, along with other general eczema treatment measures.
When you’re thinking about a molluscum contagiosum treatment for your child, it’s a good idea to weigh the costs and side effects against the possible benefits. No treatment is totally effective for this condition, so it’s possible that your child might not get the results you’re hoping for.
Preventing the spread of molluscum contagiosum
Molluscum contagiosum can spread to other places on your child’s body or to other people, including other people in your household, and other carers and children.
To reduce the spread of molluscum contagiosum to other children, don’t let your child share towels, clothes and baths.
Try to stop your child from scratching or picking at the spots. Also remember to practise good hand-washing.
If your child has molluscum contagiosum, they can keep going to child care or school.