About hives or urticaria
Hives or urticaria are smooth, raised spots that form a very itchy rash. They’re usually harmless.
Hives develop when the body releases histamines. The histamine makes small blood vessels in the skin open up and leak fluid, causing the skin surface to swell.
Hives can have several causes:
- an allergic reaction
- a viral infection, like those that cause colds or diarrhoea
- heat
- tight-fitting or scratchy clothing – this is more common if your child has eczema.
Most children develop hives for no obvious reason.
Hives are very common but not contagious.
Symptoms of hives or urticaria
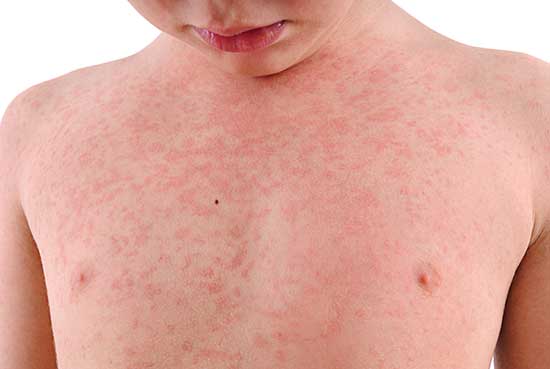
Hives look like raised spots, which are sometimes merged together. On children and teenagers with dark skin, the spots might look brown, purple or grey. On children and teenagers with light skin, the spots might look red or white.
Hives can happen anywhere on the skin, but they’re often found on the chest, stomach or back. They also tend to move around the body. For example, your child might get hives that come and go on their stomach. Then they might get hives that come and go on their arms.
Some children and teenagers might get deeper swelling in the areas where they have hives, especially on the eyelids, lips and tongue.
Hives are very itchy and can cause a burning sensation. Your child might also feel itchy in areas with no spots.
Hives can take hours or days to develop. They don’t always come up immediately after your child is exposed to a trigger like an allergen. Once they appear, they usually last from a few minutes up to 24 hours. Sometimes they keep coming back for up to 6 weeks.
When hives go, they leave no scarring.
Sometimes hives come and go for many months or years. This is known as chronic hives, and there’s usually no specific cause.
Medical help: when to get it for children and teenagers with hives or urticaria
It’s a good idea to take your child to your GP, especially if your child:
- has hives that keep coming back for longer than 6 weeks
- is itchy, uncomfortable or finding it hard to sleep because of the hives
- isn’t responding to treatment like antihistamines.
If the hives last for more than 6 weeks, your GP might refer you to a dermatologist. If the GP thinks your child’s hives are being caused by an allergy, they might refer your child to an allergy and immunology specialist.
You should take your child to your local hospital emergency department if their hives:
- cover a large area of their body
- come up very quickly after a new food, medicine, bee sting or other obvious trigger
- heal with blue or purple bruising.
Also take your child to hospital if they’re very tired or generally unwell or have a fever as well as the hives.
Sometimes hives are a sign of anaphylaxis. If your child has hives and signs of anaphylaxis, they need urgent medical attention. Signs of anaphylaxis include difficulty breathing, a swollen tongue or throat, dizziness or fainting. Here’s what to do: lay your child flat or keep them sitting. Use an adrenaline auto-injector if one is available. Call an ambulance immediately – phone 000.
Treatment for hives or urticaria
If you know what’s triggering your child’s hives, remove the trigger and stop your child from coming into contact with it in the future. This will also help to prevent hives from coming back.
Rubbing and scratching the hives will make them worse. Here’s how to relieve itching and burning:
- Put a cool face washer or towel on the hives.
- Use a fan to blow air on the skin. For safety, watch younger children and make sure they don’t put their fingers and toes too close to the fan.
- Give your child a cool shower or bath, but be careful that your child doesn’t get too cold.
- Apply calamine lotion to the hives and let it dry.
You can give your child antihistamines if your child is over 6 months. If your child is under 2 years, make sure you use a non-drowsy antihistamine. If you’re not sure which antihistamine to use, ask your pharmacist. It’s best to take the antihistamine regularly until the hives clear up completely.
In severe cases of hives, your GP might prescribe a short course of corticosteroid tablets.